Overall survival (OS) results of phase III ARAMIS study of darolutamide (DARO) added to androgen deprivation therapy (ADT) for nonmetastatic castration-resistant prostate cancer (nmCRPC)
- Abstract
- Poster Presentation
- Poster
Authors: Karim Fizazi, Neal D. Shore, Teuvo Tammela, Albertas Ulys, Egils Vjaters, Sergey Polyakov, Mindaugas Jievaltas, Murilo Luz, Boris Alekseev, Iris Kuss, Marie-Aude Le Berre, Oana Petrenciuc, Amir Snapir, Toni Sarapohja, Matthew Raymond Smith; Institut Gustave Roussy and University of Paris Sud, Villejuif, France; Carolina Urologic Research Center, Myrtle Beach, SC; Tampere University Hospital, Tampere, Finland; National Cancer Institute, Vilnius, Lithuania; Stradins Clinical University Hospital, Riga, Latvia; N.N. Alexandrov National Cancer Centre of Belarus, Minsk, Belarus; Lithuanian University of Health Sciences, Medical Academy, Kaunas, Lithuania; Hospital Erasto Gaertner, Curitiba, PR, Brazil; National Medical Research Radiological Center, Ministry of Health of the Russian Federation, Moscow, Russian Federation; Bayer AG, Berlin, Germany; Bayer HealthCare, Whippany, NJ; Orion Corporation Orion Pharma, Espoo, Finland; Massachusetts General Hospital Cancer Center, Boston, MA
Research Funding: Bayer AG and Orion Pharma
Background: DARO is a structurally distinct androgen receptor inhibitor with a favorable safety profile, approved for treating men with nmCRPC after demonstrating significantly prolonged metastasis-free survival, compared with placebo (PBO), in the phase III ARAMIS trial: median 40.4 vs 18.4 months, respectively (HR 0.41; 95% CI 0.34–0.50; P<0.0001). We report final analyses of OS and prospectively collected, patient-relevant secondary endpoints, and updated safety results.
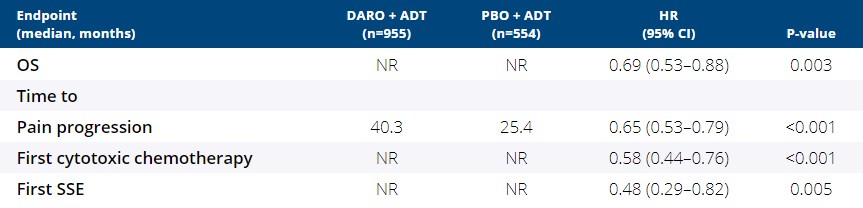
Methods: 1509 patients (pts) with nmCRPC were randomized 2:1 to DARO 600 mg twice daily (n=955) or PBO (n=554) while continuing ADT. Secondary endpoints included OS, and times to pain progression, first cytotoxic chemotherapy, and first symptomatic skeletal event. The OS analysis was planned to occur after approximately 240 deaths. Secondary endpoints were evaluated in a hierarchical order.
Results: Final analysis was conducted after 254 deaths were observed (15.5% of DARO and 19.1% of PBO patients). After unblinding at the primary analysis, 170 pts crossed over from PBO to DARO. DARO showed a statistically significant OS benefit corresponding to a 31% reduction in the risk of death compared with placebo. All other secondary endpoints were significantly prolonged by DARO (Table), regardless of the effect of crossover and subsequent therapies on survival benefit. Incidences of treatment-emergent adverse events (AEs) with ≥5% frequency were generally comparable between DARO and PBO, similar to the safety profile observed at the primary analysis. Incidences of AEs of interest (including falls, CNS effects, and hypertension) were not increased with DARO compared with PBO when adjusted for treatment exposure. AEs in the crossover group were consistent with those for the DARO treatment arm.
Conclusions: DARO showed a statistically significant OS benefit for men with nmCRPC. In addition, DARO delayed onset of cancer-related symptoms and subsequent chemotherapy, compared with PBO. With extended follow-up, safety and tolerability were favorable and consistent with the primary ARAMIS analysis (Fizazi et al, N Engl J Med 2019;380:1235-46). Clinical trial information: NCT02200614.
Poster Session – Safety outcomes of darolutamide versus apalutamide and enzalutamide in nonmetastatic castration-resistant prostate cancer (nmCRPC): Matching-adjusted indirect comparisons
Disclaimer
ASCO® and American Society of Clinical Oncology® are registered trademarks of the American Society of Clinical Oncology, Inc. Used with permission.
This selection of presentations does not necessarily represent a balanced view or full discussion of any given subject. The ideas and opinions expressed herein do not necessarily reflect those of ASCO. The authors, editors, and ASCO are not responsible for errors or omissions in translations. The mention of any company, product, service, or therapy in this collection of materials does not constitute an endorsement of any kind by ASCO. It is the responsibility of the treating physician or other health care provider, relying on independent experience and knowledge of the patient, to determine drug dosages and the best treatment for the patient. Viewers are advised to check the appropriate medical literature and the product information currently provided by the manufacturer of each drug to be administered to verify, among other matters, the dosage, method, and duration of administration, or contraindications. Viewers are also encouraged to contact the manufacturer with questions about the features or limitations of any products. ASCO assumes no responsibility for any injury or damage to persons or property arising out of or related to any use of the material contained in this publication or to any errors or omissions.
Copyright © 2020 Springer Healthcare Limited. Part of the Springer Nature Group.
PP-M_DAR-NL-0021-1